Vasculitis
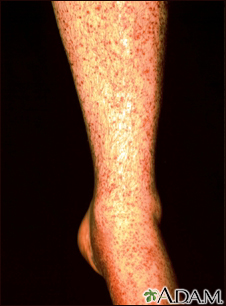
What is Vasculitis?
Vasculitis refers to a group of rare autoimmune disorders characterized by inflammation of the blood vessels. In vasculitis, the immune system mistakenly attacks the blood vessels, causing them to become swollen, narrowed, or damaged. This can lead to restricted blood flow to organs and tissues, resulting in a range of symptoms depending on the type and location of the affected blood vessels. Vasculitis can affect any organ in the body and may be acute or chronic.
Who's at risk for Vasculitis?
Vasculitis can affect individuals of all ages, genders, and ethnic backgrounds. The exact cause of vasculitis is often unknown, but certain factors may increase the risk of developing the condition:
- Autoimmune disorders: Individuals with autoimmune disorders, such as rheumatoid arthritis or lupus, may have a higher risk of developing vasculitis.
- Infections: Some infections, such as hepatitis B or hepatitis C, may trigger vasculitis in susceptible individuals.
- Medications: Certain medications, such as antibiotics or nonsteroidal anti-inflammatory drugs (NSAIDs), have been associated with the development of vasculitis in some cases.
- Genetic factors: There may be a genetic predisposition to developing vasculitis, as it can sometimes run in families.
- Environmental triggers: Exposure to certain environmental factors, such as chemicals or pollutants, may contribute to the development of vasculitis in susceptible individuals.
What causes Vasculitis?
The exact cause of vasculitis is often unknown or multifactorial. In many cases, it is believed to be an autoimmune response, where the immune system mistakenly attacks the blood vessels. However, the trigger for this abnormal immune response is often unclear. It is thought that a combination of genetic, environmental, and immunological factors may play a role in the development of vasculitis. In some cases, infections, medications, or other underlying medical conditions may act as triggers for vasculitis.
How does Vasculitis start?
Vasculitis can start with the activation of the immune system, leading to inflammation and damage to the blood vessels. The specific mechanisms vary depending on the type of vasculitis and the affected organs. Inflammation can cause the blood vessels to become swollen, narrowed, or blocked, leading to restricted blood flow. This can result in a wide range of symptoms and complications, depending on which organs or tissues are affected.
What are the symptoms of Vasculitis?
The symptoms of vasculitis can vary depending on the type of vasculitis and the organs or tissues affected. Common symptoms may include:
- Fatigue and malaise: Many individuals with vasculitis experience a general feeling of fatigue, weakness, or malaise.
- Fever: Some types of vasculitis can cause persistent or recurrent fever.
- Joint and muscle pain: Joint and muscle pain, stiffness, and swelling may occur in some individuals.
- Skin changes: Skin rash, ulcers, or nodules may develop in certain types of vasculitis.
- Nerve problems: Vasculitis can affect the nerves, leading to symptoms such as numbness, tingling, weakness, or shooting pain.
- Organ-specific symptoms: Depending on the organs affected, individuals may experience symptoms such as shortness of breath, cough, chest pain, abdominal pain, gastrointestinal bleeding, or kidney problems.
It's important to note that the symptoms of vasculitis can be similar to those of other conditions, and diagnosis requires a thorough evaluation by a healthcare professional.
How is Vasculitis diagnosed?
Diagnosing vasculitis involves a combination of medical history review, physical examination, laboratory tests, and imaging studies. The specific diagnostic approach may vary depending on the suspected type of vasculitis and the organs involved. The following tests and procedures may be conducted:
- Blood tests: Blood tests can help detect inflammation markers, evaluate organ function, and identify specific antibodies associated with certain types of vasculitis.
- Biopsy: In some cases, a small sample of affected tissue, such as the skin, muscle, or organ, may be taken for microscopic examination to confirm the presence of vasculitis and determine the type.
- Imaging studies: Imaging tests, such as X-rays, ultrasound, computed tomography (CT), or magnetic resonance imaging (MRI), may be used to visualize blood vessels and assess organ involvement.
- Angiography: Angiography involves injecting a contrast dye into the blood vessels and taking X-rays or performing other imaging techniques to evaluate the blood flow and detect any abnormalities.
A multidisciplinary approach involving specialists such as rheumatologists, dermatologists, nephrologists, or pulmonologists may be necessary for an accurate diagnosis.
How can Vasculitis be treated?
The treatment of vasculitis aims to reduce inflammation, control symptoms, prevent organ damage, and manage complications. The specific treatment approach depends on the type and severity of vasculitis and may include:
- Medications: Immunosuppressive medications, such as corticosteroids, may be prescribed to suppress the abnormal immune response and reduce inflammation. Other immunosuppressive drugs, such as methotrexate, azathioprine, or rituximab, may be used in certain cases. Nonsteroidal anti-inflammatory drugs (NSAIDs) or analgesics may be recommended for pain relief.
- Disease-modifying antirheumatic drugs (DMARDs): DMARDs, such as methotrexate or azathioprine, may be used to control inflammation and prevent disease flares in certain types of vasculitis.
- Biologic therapies: Biologic drugs, such as rituximab or tocilizumab, may be prescribed for severe or refractory cases of vasculitis.
- Supportive care: Depending on the organ involvement and symptoms, supportive measures may be employed, such as pain management, physical therapy, or occupational therapy.
- Lifestyle modifications: Healthy lifestyle habits, including regular exercise, a balanced diet, and stress management, can support overall health and well-being.
The treatment plan should be tailored to the individual's specific condition and may require close monitoring and periodic adjustments.
What complications may occur with Vasculitis?
Vasculitis can lead to various complications depending on the type and severity of the disease. Complications may include:
- Organ damage: Chronic or severe vasculitis can lead to damage or dysfunction of the affected organs, such as the lungs, kidneys, heart, or nervous system.
- Increased infection risk: Some medications used to treat vasculitis can suppress the immune system, increasing the risk of infections.
- Blood vessel complications: Inflammation of the blood vessels can cause narrowing, blockages, or aneurysms, which can lead to reduced blood flow or vessel rupture.
- Secondary conditions: Individuals with vasculitis may be at an increased risk of developing other autoimmune disorders or conditions, such as heart disease or blood clots.
How can I prevent Vasculitis?
As the causes of vasculitis are not fully understood, it is challenging to prevent the condition. However, early detection, prompt treatment, and ongoing medical care can help manage symptoms, reduce complications, and improve the overall quality of life for individuals with vasculitis. It's important to work closely with a healthcare professional to develop an appropriate management plan.
Where can I go for more information on Vasculitis?
For more information on vasculitis, reliable sources such as the Vasculitis Foundation, American College of Rheumatology, and Mayo Clinic can provide valuable information and resources. Consulting with a healthcare professional, such as a rheumatologist or primary care physician, can also provide personalized information and guidance specific to an individual's situation.

