Dialysis
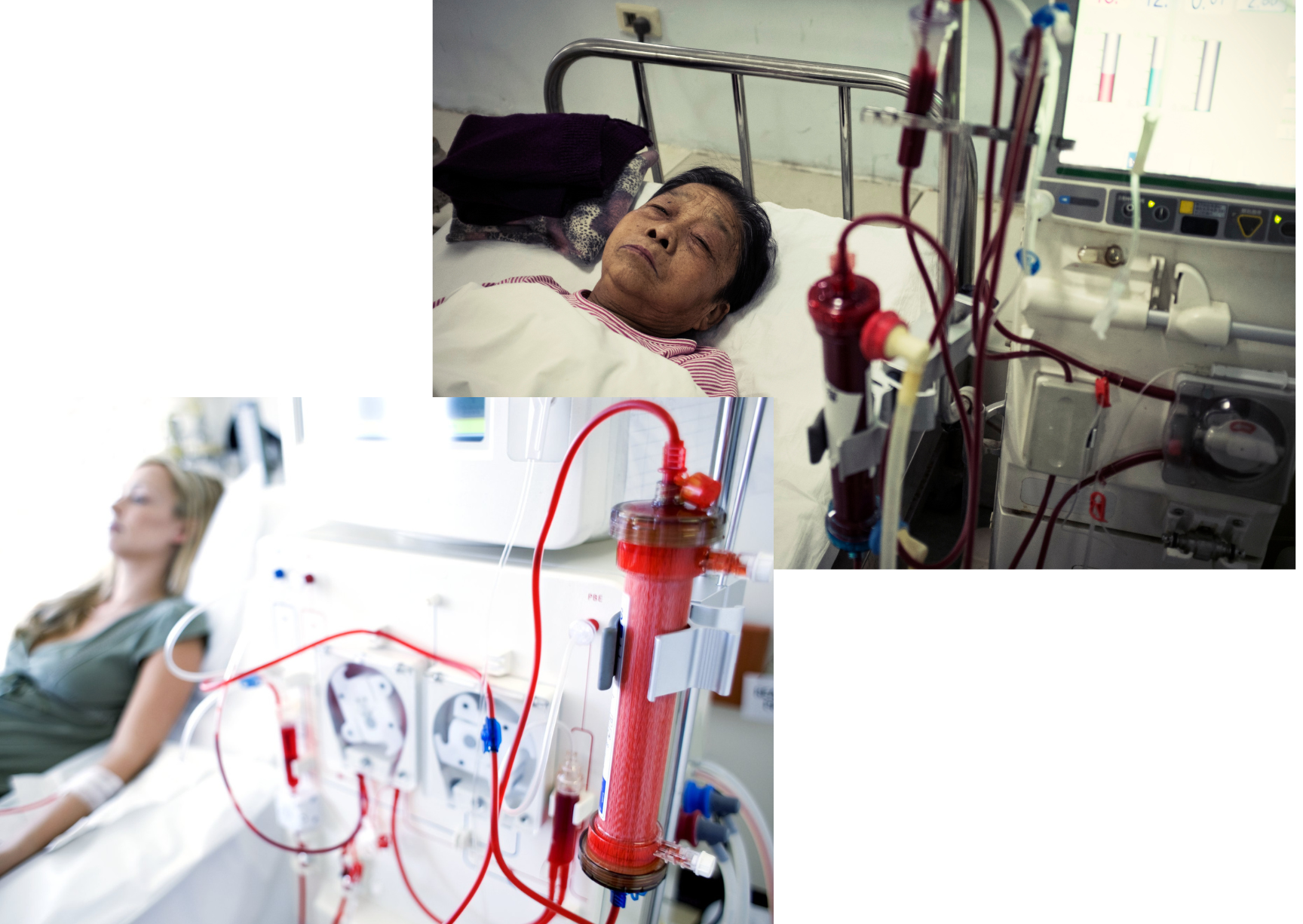
Dialysis is a life-saving treatment for individuals with kidney failure. In this article, we will address common questions about dialysis, including its purpose, risk factors, types, potential complications, and long-term management.
What is dialysis?
Dialysis is a medical procedure that artificially removes waste products, excess fluids, and electrolytes from the blood when the kidneys are unable to do so due to kidney failure. It serves as a replacement for lost kidney function and helps maintain the body's chemical balance.
Who’s at risk for needing dialysis?
Individuals with chronic kidney disease (CKD), especially those in the advanced stages or with end-stage renal disease (ESRD), are at risk for needing dialysis. Other risk factors include:
- Diabetes
- High blood pressure
- Family history of kidney disease
- Age, as kidney function tends to decline with age
- Ethnicity, with a higher prevalence in African Americans, Hispanics, and Native Americans
What causes the need for dialysis?
The need for dialysis arises when the kidneys can no longer adequately filter waste products and maintain the body's chemical balance due to kidney failure. Common causes of kidney failure include:
- Diabetes, the leading cause of kidney failure in many countries
- Hypertension (high blood pressure)
- Glomerulonephritis, an inflammation of the glomeruli in the kidneys
- Polycystic kidney disease, a genetic disorder causing multiple cysts in the kidneys
- Lupus and other autoimmune diseases
How does the need for dialysis start?
The need for dialysis starts when the kidneys' ability to filter waste and excess fluids from the blood declines progressively due to kidney disease or damage. When kidney function drops below a certain threshold (typically around 10-15% of normal function), dialysis becomes necessary to remove waste products and maintain electrolyte balance.
What are the symptoms indicating the need for dialysis?
Symptoms indicating the need for dialysis may include:
- Severe fatigue and weakness
- Shortness of breath
- Swelling in the face, hands, feet, or abdomen (edema)
- Nausea and vomiting
- Loss of appetite
- Persistent itching
- Confusion and difficulty concentrating
How is the need for dialysis diagnosed?
The need for dialysis is determined by evaluating kidney function through blood tests, such as estimated glomerular filtration rate (eGFR) and serum creatinine levels. Additional tests, such as urinalysis and imaging studies, may also be performed to assess kidney damage and function.
How can dialysis be performed?
There are two main types of dialysis:
Hemodialysis: Blood is filtered through an artificial kidney machine (dialyzer) outside the body, and cleaned blood is returned to the patient. Hemodialysis is typically performed three times a week at a dialysis center.
Peritoneal dialysis: A catheter is inserted into the abdomen, and a dialysis solution is used to absorb waste products and excess fluids from the blood through the peritoneal membrane. The used solution is then drained and replaced with fresh solution.
Peritoneal dialysis can be performed at home daily.
What complications may occur with dialysis?
Complications associated with dialysis can include:
- Infection, particularly at the site of the catheter or vascular access
- Low blood pressure during hemodialysis sessions
- Anemia due to reduced production of erythropoietin by the kidneys
- Mineral and bone disorders, such as secondary hyperparathyroidism and renal osteodystrophy
- Emotional and mental health challenges, including anxiety and depression
How can I prevent the need for dialysis?
Preventing the need for dialysis primarily involves managing and controlling the risk factors for kidney disease. Some prevention strategies include:
- Maintaining a healthy diet, low in salt and processed foods
- Regular exercise and maintaining a healthy weight
- Controlling blood sugar levels if you have diabetes
- Monitoring and managing high blood pressure
- Avoiding excessive use of nonsteroidal anti-inflammatory drugs (NSAIDs) and other medications that can harm the kidneys
- Quitting smoking
- Regular check-ups and kidney function tests for those at risk
Long-term management of dialysis
Long-term management of dialysis requires ongoing medical care and coordination with a healthcare team, including nephrologists, dialysis nurses, and dietitians. Key aspects of long-term management include:
- Adherence to the dialysis schedule
- Monitoring and adjusting medications as needed
- Maintaining a kidney-friendly diet and fluid restrictions
- Regular blood tests to monitor electrolyte levels and anemia
- Emotional and mental health support, such as counseling or support groups
What is recent research saying about dialysis?
Recent research on dialysis has focused on improving treatment options, developing more efficient dialysis machines, and exploring alternative therapies, such as bioartificial kidneys and stem cell treatments. Studies have also investigated the impact of various dialysis modalities on patient outcomes, including quality of life, cardiovascular health, and mortality rates. Additionally, research continues to explore ways to improve access to care and reduce disparities in dialysis treatment and outcomes.
Where can I go for more information on dialysis?
For more information on dialysis or support, consider reaching out to your healthcare provider or a qualified medical professional. They can provide guidance based on your specific situation and answer any questions you may have. Reputable online resources, such as the National Kidney Foundation, the American Association of Kidney Patients, and the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), can also offer valuable information and support for those affected by kidney disease and requiring dialysis.

