Thrush
What is Thrush?
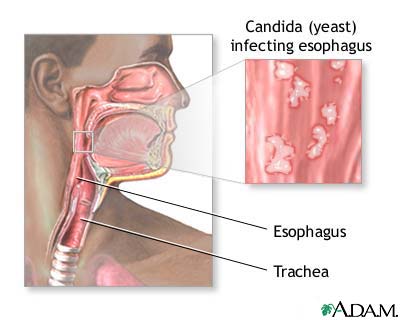
Thrush, also known as oral candidiasis, is a fungal infection caused by Candida yeast. It commonly affects the mouth and throat, causing white or creamy lesions on the tongue, inner cheeks, roof of the mouth, and throat. Thrush can occur in people of all ages, but it is more common in infants, older adults, and individuals with weakened immune systems.
Who's at risk for Thrush?
Certain factors increase the risk of developing thrush. Infants are prone to thrush due to their developing immune systems and limited ability to control the growth of yeast. Older adults may be more susceptible due to age-related changes in immune function and underlying health conditions. Individuals with weakened immune systems, such as those with HIV/AIDS, undergoing chemotherapy, or taking immunosuppressive medications, are at a higher risk. Other risk factors include diabetes, poor oral hygiene, smoking, and the use of dentures or mouth appliances that can promote yeast overgrowth.
What causes Thrush?
Thrush is caused by an overgrowth of the Candida yeast, typically Candida albicans, in the mouth and throat. Candida is a normal part of the oral flora, but an imbalance can lead to its overgrowth and the development of thrush. Factors that disrupt the natural balance of microorganisms in the mouth, such as weakened immune function, can allow Candida to multiply and cause infection. Additionally, certain medications, such as antibiotics or corticosteroids, can increase the risk of developing thrush by altering the oral microbiota.
How does Thrush start?
Thrush typically starts when the Candida yeast overgrows in the mouth and throat. The yeast can proliferate due to factors that disturb the natural balance of microorganisms in the oral cavity. This imbalance may be triggered by factors such as weakened immune function, antibiotic use, corticosteroid use, or underlying health conditions. The overgrowth of Candida leads to the development of white or creamy patches in the mouth and throat, which characterize the condition.
What are the symptoms of Thrush?
The symptoms of thrush can vary but commonly include white or creamy lesions on the tongue, inner cheeks, gums, tonsils, or throat. These lesions may resemble cottage cheese and can be easily scraped off, leaving a red or raw area underneath. Other symptoms may include pain or discomfort while eating or swallowing, a dry or cottony feeling in the mouth, altered taste sensation, a burning sensation, and in severe cases, cracking or redness at the corners of the mouth.
How is Thrush diagnosed?
Thrush is typically diagnosed through a visual examination of the mouth and throat by a healthcare professional. The characteristic appearance of white or creamy lesions on the mucous membranes is often sufficient to diagnose thrush. In some cases, a sample of the affected tissue may be taken for laboratory testing to confirm the presence of Candida yeast. Additional diagnostic tests may be recommended if the thrush is recurrent or does not respond to standard treatments.
How can Thrush be treated?
Treatment of thrush usually involves antifungal medications to eliminate the Candida yeast. These medications can be in the form of oral rinses, gels, lozenges, or systemic antifungal drugs, depending on the severity and location of the infection. It is important to complete the full course of treatment as prescribed by a healthcare professional, even if symptoms improve before the medication is finished. Good oral hygiene practices, such as regular brushing of teeth and tongue cleaning, may also be recommended.
What complications may occur with Thrush?
In most cases, thrush is a mild and easily treatable condition. However, if left untreated or if the immune system is severely compromised, the infection can spread to other parts of the body, leading to systemic candidiasis. Systemic candidiasis is a more serious condition that can affect vital organs and may require more aggressive treatment. Individuals with weakened immune systems, such as those with HIV/AIDS or undergoing chemotherapy, are at a higher risk of developing systemic candidiasis.
How can I prevent Thrush?
To help prevent thrush, maintaining good oral hygiene is essential. This includes regular brushing of teeth, cleaning the tongue, and using an antifungal mouthwash if recommended by a healthcare professional. It is important to follow proper denture care practices and remove dentures at night to allow the mouth to rest and be properly cleaned. Individuals with underlying health conditions that weaken the immune system should work closely with their healthcare provider to manage their condition and minimize the risk of thrush.
Long-term management of Thrush
For individuals with recurrent or persistent thrush, long-term management may involve identifying and addressing underlying causes or contributing factors. This may include managing any underlying health conditions, optimizing immune function, and reviewing medications that may increase the risk of thrush. Regular follow-up appointments with a healthcare professional may be necessary to monitor the condition, adjust treatment as needed, and ensure proper oral health practices are being followed.
What is recent research saying about Thrush?
Recent research on thrush has focused on understanding the mechanisms of Candida overgrowth and identifying potential new treatment options. Scientists are studying the interactions between Candida and the immune system to develop more targeted approaches to prevent and treat thrush. Additionally, research is ongoing to explore the role of probiotics and other interventions that may help restore the balance of microorganisms in the mouth and prevent the recurrence of thrush.
Where can I go for more information on Thrush?
For more information on thrush, reputable sources such as the American Academy of Oral Medicine (AAOM), American Dental Association (ADA), or the National Institute of Dental and Craniofacial Research (NIDCR) can provide valuable information and resources. These organizations offer reliable information on thrush, including prevention strategies, treatment options, and support networks. Consulting with a healthcare professional, such as a dentist or primary care provider, can also provide personalized information and guidance specific to an individual's situation.

